A little pink in the sink is not something to ignore. In many cases, bleeding gums are an early sign of inflammation caused by plaque buildup.
A lot of people stop flossing the moment they see blood. That feels logical, but it is usually the opposite of what your gums need. Most of the time, bleeding happens because bacteria and plaque have been sitting around the gumline and between the teeth, irritating the tissue day after day.
We are going straight to the point, no jargon, just clear answers. Here are the most common reasons your gums bleed

Let's discover it!
1. The Most Common Cause: Plaque Buildup
The number one reason gums bleed is simple: plaque.
Plaque is a sticky film of bacteria that forms on your teeth every day. If it is not removed thoroughly, it collects near the gumline and between teeth. Over time, your gums become irritated, swollen, and more likely to bleed during brushing or flossing.
Regular checkups and cleanings are one of the best ways to catch and reverse this early.
If plaque stays in place too long, it hardens into tartar. Once tartar forms, you cannot brush it off at home. That is where professional cleanings come in. A routine preventative dentistry visit helps remove that hardened buildup and gives your gums a chance to heal.
2. You Might Not Be Flossing Enough
REMEMBER: Your toothbrush cannot reach the tight spaces between teeth very well.
If food and bacteria stay there, the gums become inflamed and start bleeding when floss finally reaches them.
This is why so many people say, “My gums bleed every time I floss,” when the real issue is often that they do not floss consistently enough.
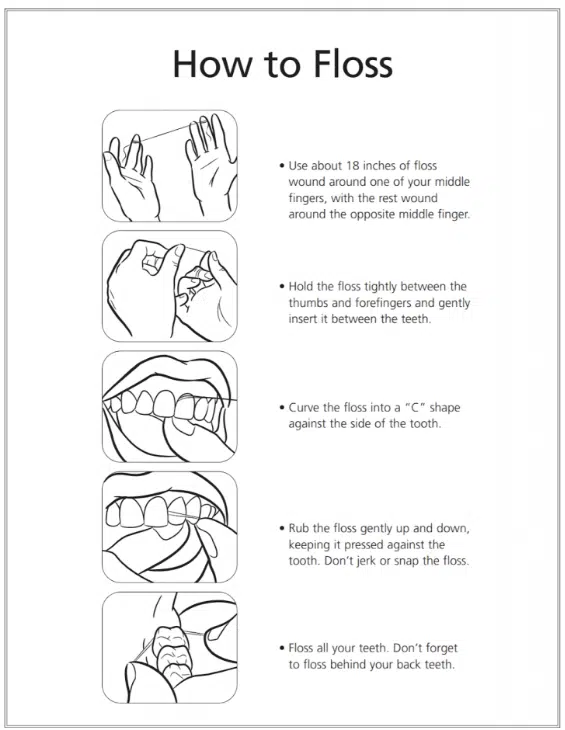
SOLUTION: If this sounds like you, do not panic. In many cases, if you floss gently but consistently once a day, the bleeding starts improving within about a week or two. The key is to be gentle but thorough. Slide the floss under the gumline, curve it around each tooth in a “C” shape, and clean both sides of the space.
If you are not sure whether your technique is right, that is something your hygienist can show you during preventive care.
3. You Could Be Brushing Too Hard
Bleeding gums are not always about not cleaning enough. Sometimes, it is about brushing too aggressively.
A lot of people think scrubbing harder means cleaner teeth. It does not. Harsh brushing can irritate the gums, wear away enamel, and even cause gum recession over time. If you use a hard-bristled brush or scrub back and forth fast, your gums may bleed simply because they are being traumatized every day.
What to do instead:
- Use a soft-bristled toothbrush
- Hold it gently, not with a tight fist
- Brush with small circular motions
- Angle the bristles toward the gumline instead of attacking the gums directly
If your gums are sore, swollen, or starting to pull back, it is smart to mention it at your next checkup and cleaning.
4. Gingivitis Can Turn Into Bigger Problems
Bleeding gums are often the first warning sign of gingivitis. If gingivitis is ignored, it can progress into more serious gum disease. At that point, the inflammation can start affecting the bone and support around the teeth, not just the soft tissue.
That means what started as “a little bleeding” can eventually turn into:
- chronic bad breath
- gum recession
- loose teeth
- discomfort when chewing
- deeper cleanings or more involved treatment
That is exactly why you should not shrug this off. If your gums bleed regularly, this is your sign to do something now. Early treatment is easier, faster, and much less expensive than waiting until there is real damage. Regular exams and preventative dentistry are designed to stop problems at this early stage.
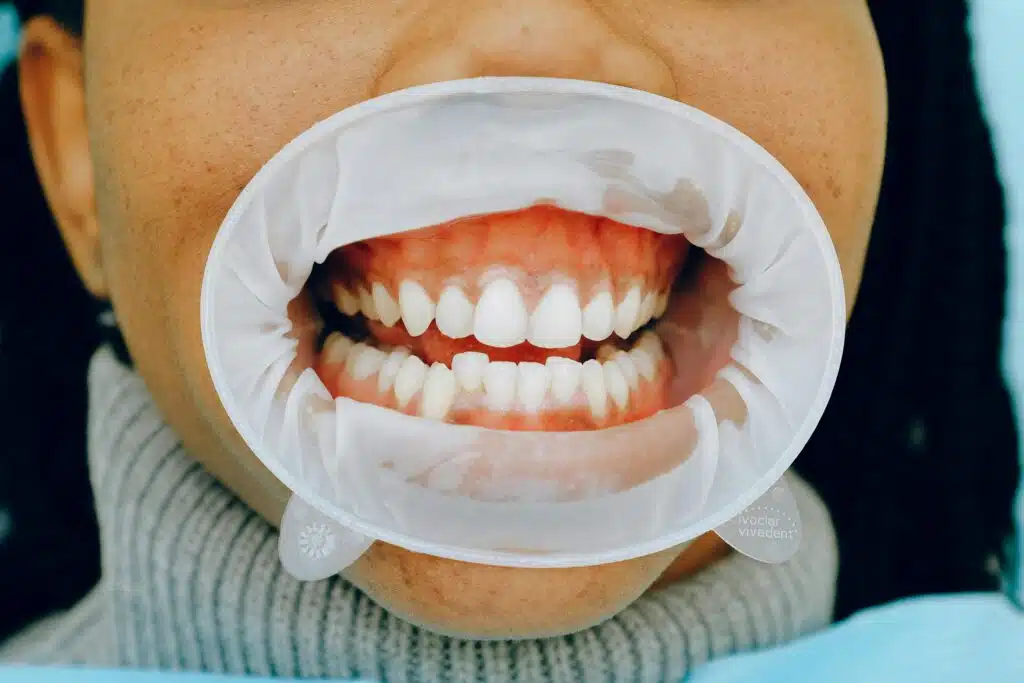

5. Crooked Teeth Can Make Gums Bleed More Easily
If your teeth are crowded or overlapping, certain areas may be harder to clean. That means plaque builds up faster, especially near the gums and between teeth. Even people with good brushing habits can struggle if the alignment makes access difficult.
That is one reason why straighter teeth are often easier to keep healthy. If your bleeding seems to happen in the same tight areas over and over, an evaluation for orthodontics and clear aligners may be worth discussing.
This does not mean everyone with bleeding gums needs orthodontic treatment. It just means the physical shape and spacing of your teeth may be part of the problem.
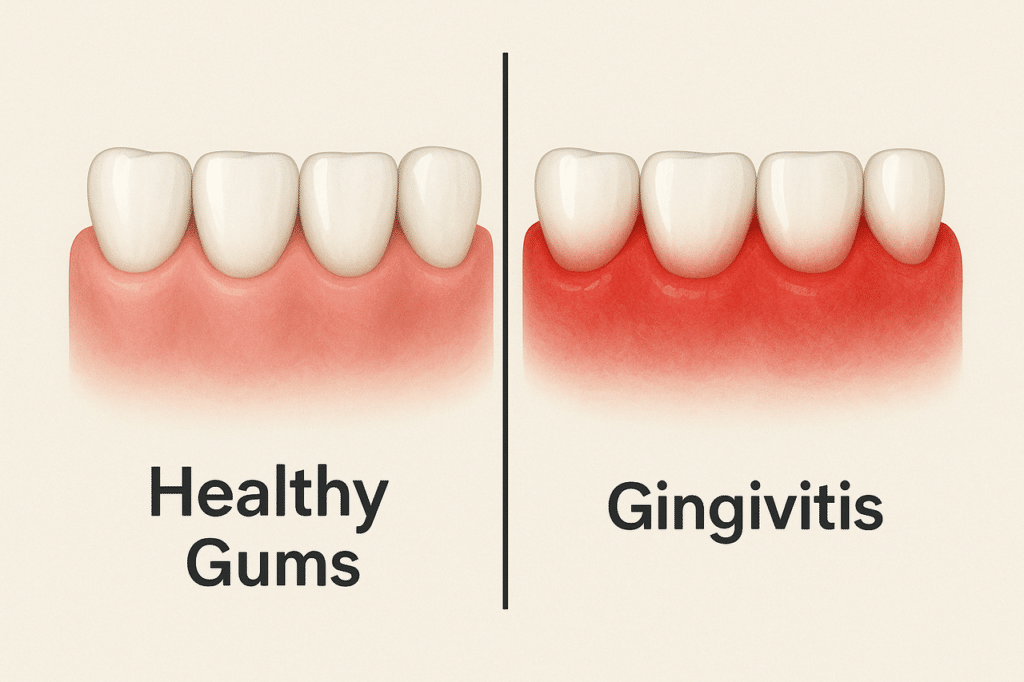
3) Gum Inflammation and Early Infection
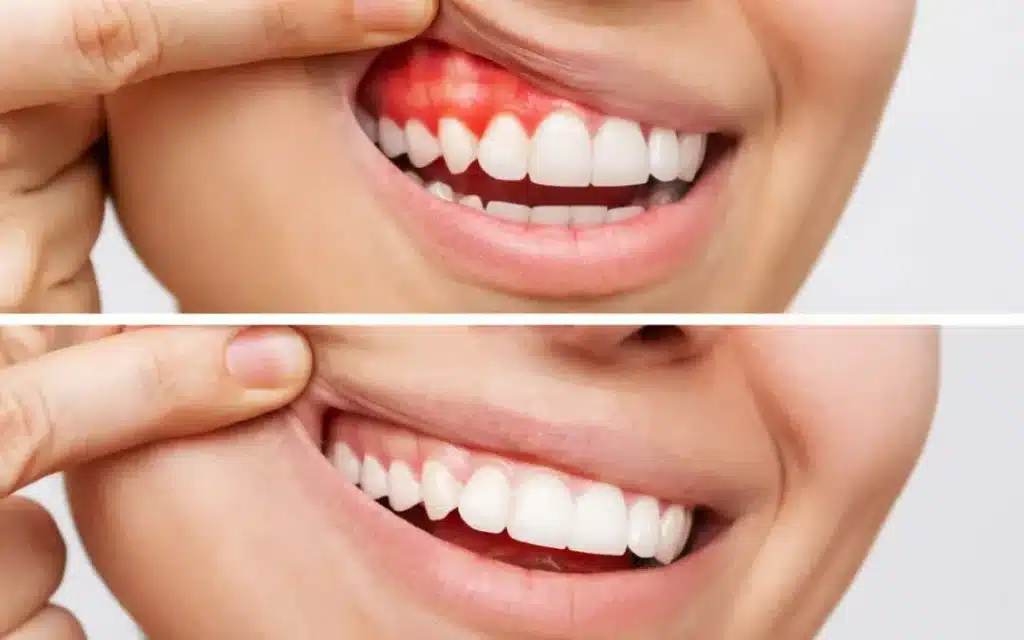
Inflamed gums (gingivitis) and early periodontal problems trap bacteria under the gumline, creating a constant source of sulfur odors. You might notice tenderness, bleeding when brushing.
Fix it:
- This is urgent, you have to schedule a professional evaluation and targeted cleaning during routine checkups. Catching inflammation early is the fastest way to reverse it.
- Use a soft brush at a 45-degree angle toward the gums with short, gentle strokes.
- Never skip flossing—this is where gum healing usually starts.
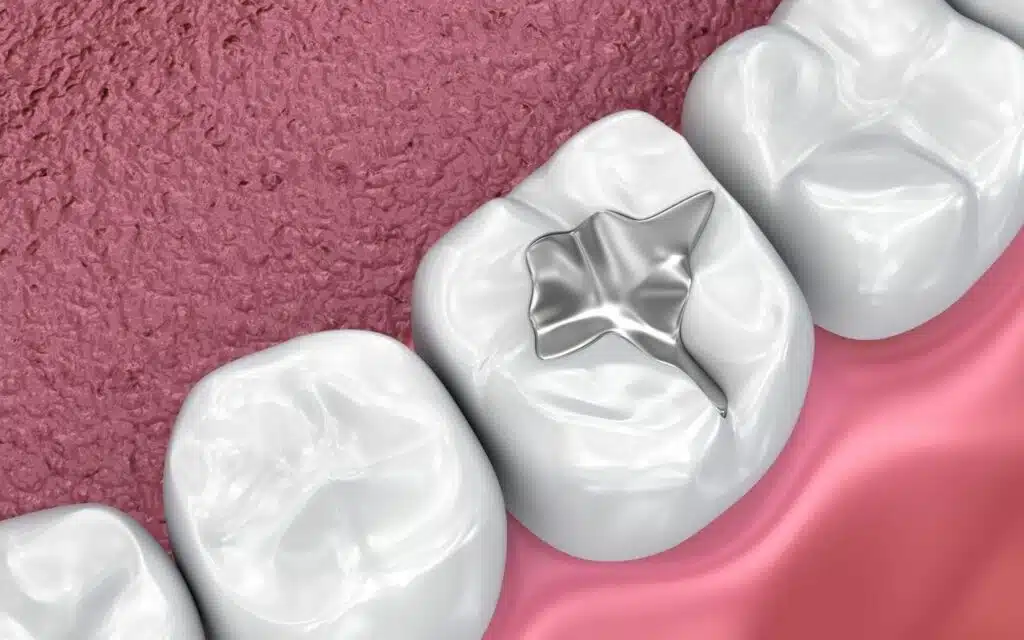
4) Cavities, Broken Fillings, and Food Traps
A cavity or a rough, broken edge on a filling becomes a pocket that holds food and bacteria—exactly what causes bad breath. Crowded teeth can create similar traps.
Fix it:
- Ask for a focused exam and bite-wing X-rays at your next general & cosmetic dentistry visit to find hidden traps and repair them conservatively.
- If a tooth is weakened or fractured, a durable crown can seal out bacteria and restore function—often the same day with CEREC.
- Persistent crowding that traps food between teeth may benefit from clear aligners to improve spacing and hygiene access.
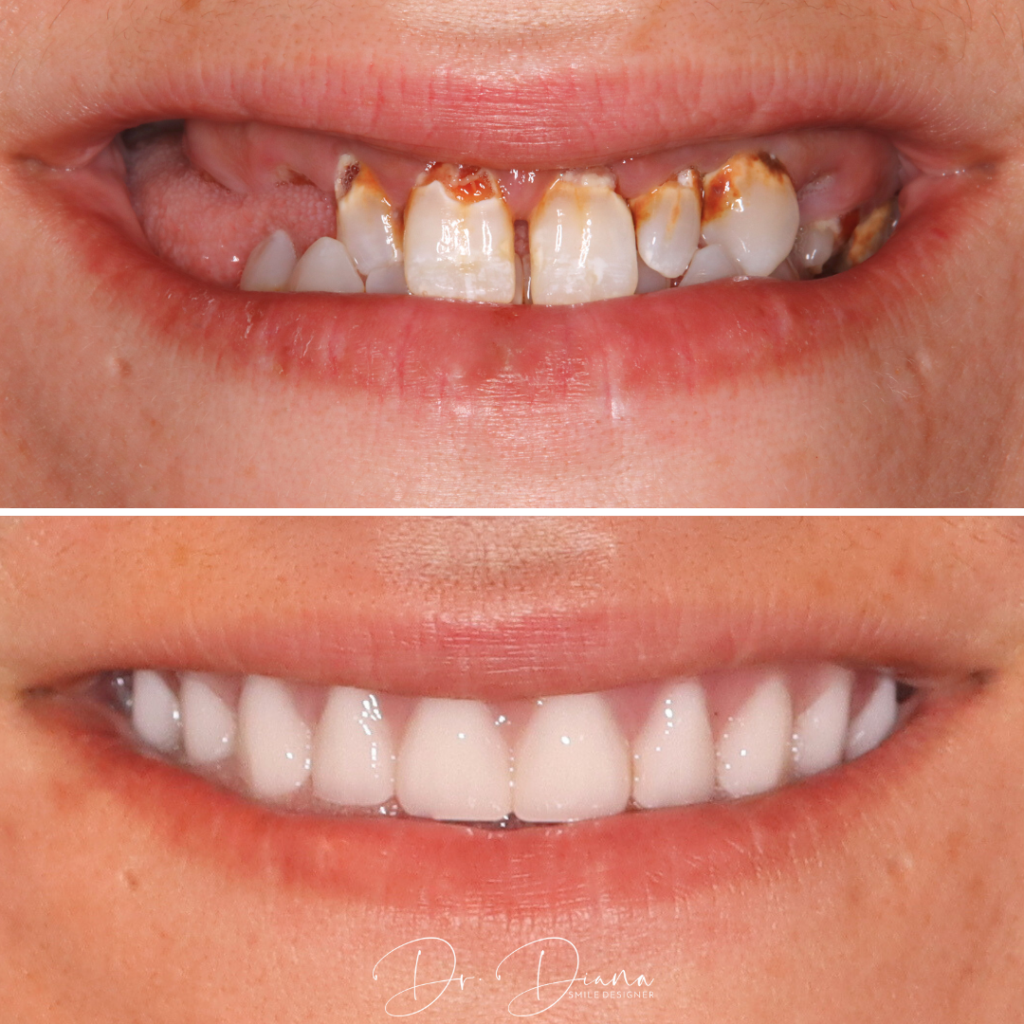
5) When a Tooth Can’t Be Saved
Advanced decay, fractures below the gumline, or severe periodontal disease can create chronic odor that brushing won’t solve. In these cases, definitive treatment may include removing the problem tooth and replacing it.
Fix it:
- Your dentist will review options; when replacement is needed, modern dental implants restore function and appearance and are easier to keep clean than older options.
A Simple At-Home Breath Reset (7-Day Plan)
Day 1–2: Deep Clean & Reset
- Replace your toothbrush head (or switch to soft-bristle if you scrub hard).
- Commit to the full routine twice daily: brush 2 minutes, floss, and scrape your tongue.
- Drink water with each meal and between meals.
Day 3–4: Dry Mouth & Diet
- Cut back on alcohol-based mouthwash and add xylitol gum after meals.
- Move coffee and soda to mealtimes only; stop all-day sipping.
Day 5–6: Target Trouble Spots
- Pay attention to areas that bleed or trap food—floss there first.
- Use an interdental brush where floss shreds or feels tight.
Day 7: Maintenance Plan
- If odors persist, book a professional cleaning and exam to rule out gum disease, cavities, or broken restorations.
Frequently Asked Parent Questions
Q1: Does mouthwash cure bad breath?
It can temporarily mask odors. If breath improves only for an hour, you likely need a cleaning, tongue care, or treatment for gum inflammation during preventative visits.
Q2: Could it be my sinuses or reflux?
Yes—post-nasal drip and GERD can contribute. Solve the oral hygiene basics first; if odor persists, discuss medical causes with your dentist and primary care provider.
Q3: My teen has bad breath with braces—what helps?
Orthodontic appliances trap more plaque. Step up hygiene (interdental brushes, water flosser) and keep cleanings on schedule. If aligners are in use, ask how to clean trays to prevent odors..
Fix the Source, Not Just the Smell
Bad breath usually has a clear cause and a clear solution. Clean the places bacteria hide, keep saliva flowing, repair traps like cavities or broken fillings, and maintain regular professional care.
If you’ve tried the basics and the odor keeps returning, it’s time for a closer look and a tailored plan.
Have questions or ready to book your next visit?
Contact us today—we'll help you identify the cause and get your breath fresh again.



